By Jock Hoffman, CRICO
The shortage of
primary care physicians (PCP) in the U.S., paired with the drive to
lower costs, is challenging access to health care. One idea increasingly
advocated is granting greater responsibility and independence for the burgeoning population of nurse practitioners (NP). Scope-of-practice laws vary widely by state—from tight restriction to full independence. Physicians opposed to full independence argue, however, that that solution will bring the level of care those patients receive below a tolerable standard.
Is this just a turf battle or a patient safety debate?
Unfortunately, any focus on potential risks posed by mid-level
providers’ (NPs, physician assistants, etc.) detracts attention from
their predominately positive role in patient safety. In conjunction with
increasing access to care, non-physicians are often able to perform
tasks that physicians too short on time simply can’t get to: updating
histories, checking medication compliance, listening to secondary
complaints, providing education, etc. These activities clearly enhance
the quality of care—especially in communities with PCP shortages. Those
interactions also reduce the likelihood of miscommunication, missed
appointments, fumbled test results, unresolved complaints, and myriad
other issues that often presage an adverse event and a malpractice
allegation.
Certainly, a patient whose needs exceed the capabilities, comfort
level, or authority of a non-physician should be seen by a physician as
soon as possible. Establishing and enforcing the criteria for such
escalations is essential to protect both patients and providers. Indeed,
those criteria are the focus of the debate about whether or not
expanding the practice scope of mid-level providers increases their
patients’ vulnerability to misdiagnosis or mismanaged treatment.
Whatever rules are in place, not all patients will fully comprehend
the capabilities or limits of a non-physician they see in their doctor’s
exam room or the Emergency Department or an in-store
clinic. Quickly and sincerely addressing the concerns of such patients
will help reduce misaligned expectations. Of course, mid-level providers
are not immune to being named in malpractice claims, and those who
supervise them, generally speaking, will also be held accountable for
their care.
CRICO’s data indicate that since 2002, 75 malpractice claims or suits
cases named 83 NPs or PAs as defendants,* a rate of about one defendant
per 200 practitioners per year. Analysis of those 75 cases indicates
that inadequate supervision of the mid-level providers was identified in
19 (25%). The average incurred loss for cases involving mid-level
provider defendants was $330,000.
Supervising physicians are obliged to know (and share) what risks
these arrangements may pose to their patients and practice. Mid-level
providers without independent access to patient safety-related education
will be reliant on their colleagues and supervising MDs for alerting
them to common hazards and practice-specific concerns. As with most
learning situations, point-of-care guidance and training will have a
longer-lasting impact. Physicians and those they supervise who establish
in situ opportunities to address known or potential risks will likely
fare better than those who leave this to chance or individual
motivation.
*Mid-level provider defendants who are employed by a CRICO-insured
organization receive the same level of coverage and full complement of
benefits afforded to CRICO-insured physicians.
Additional Materials
Original Source, Strategies for Patient Safety
By Jock Hoffman, CRICO
Carving out time for patient safety education and training is a
challenge. The pressures of day-to-day practice can detract your time
and attention …until something bad happens—to a colleague, or in your
own practice. Of course, physicians who do find the time to learn how to
reduce their risk of patient harm and an allegation of malpractice, are more likely to avoid those circumstances.
In Massachusetts*, CRICO’s philosophy is reinforced by the Board
of Registration in Medicine’s Continuing Professional Development
(formerly Continuing Medical Education/CME) requirements, which dictate specific education categories, including risk management study:
Physicians must accrue 10 credits of risk management study
every two years. Four credits must be in Category 1. The additional six
credits may be in Category 1 or Category 2 risk management study.
Risk management study must include instruction in
medical malpractice such as patient safety and loss prevention.
Activities that meet these criteria may include courses in quality
assurance, bioethics, end-of-life care studies, opioid and pain
management, as well as non-economic aspects of practice management. All
of CRICO’s CME activities are designed to be suitable for risk
management study, including our newest publication, Insight and our podcasts. CRICO’s most recent issue, Insight into Communication Challenges,
offers actionable data, expertise, and personal physician perspectives
on this universal area of risk. The Massachusetts Board of Registration
in Medicine has endorsed Insight and our podcasts for Category 1 credit.
As a CRICO-insured physician, you can find help meeting these requirements through our website.
CRICO is proud to be accredited by the Accreditation Council for
Continuing Medical Education. We work side-by-side with a network of
Harvard experts to develop activities designed to help you decrease
patient harm. Of course, the Risk Management or Patient Safety departments at the hospitals and other organizations you work with—or for—also offer opportunities for CME and Risk Management credits.
No matter where you chose to go for quality patient safety and risk
management education and training, it is certain to beat trial and
error.
Additional Material
By Jock Hoffman, CRICO
As we encourage patients to be more engaged,
we may also see more who go beyond assertive to demanding care
unsupported by good clinical judgment. Understandably, physicians worry
that saying “no” to a patient increases their risk of being disliked,
dismissed, or even sued for medical malpractice. But the right mix of
clinical judgment, bedside manner, and documentation can help take the
“maybe” out of saying no to a request for unnecessary—or unsafe—testing
or treatment.
More transparency in health care means patients are more aware of
options for screening, testing, procedures, and medications—often via
direct campaigns. The advent of social media further expands the spread
of both legitimate and untrustworthy
health care information. Thus, an anxious or desperate patient may ask
for something about which they have heard or read, e.g., an MRI after a
negative mammogram, a better drug for acid reflux, a cesarean section
scheduled for convenience, an experimental procedure “like on House,
MD.” In the face of such requests, maintaining an effective patient
relationship, practicing appropriate care, and heeding the pressure to
control cost—can be a real challenge.
If your clinical judgment is to say no, then saying yes—because it is
easier, faster, less of a hassle—may pose hazards to both you and your
patient. Even relatively benign procedures can carry the risk of
unintended consequences. For example: changing a medication regimen can
destabilize a patient's health; a “convenience” delivery before 39-weeks
gestation may violate clinical guidelines
(or hospital policy); experimental procedures (even those from the real
world) are the purview of those physicians working to perfect a new
technique with patients selected via exacting criteria—not just foot
stomping.
Explaining to a patient the reasons behind “no” takes time and
patience. But thoughtfully discussing and documenting such requests will
improve your chances of maintaining good rapport and leave you less
vulnerable to an allegation of malpractice than if your refusal is curt,
dismissive, or poorly documented. Listening with respect to what the
patient's aunt or neighbor or favorite blogger has suggested gives you
an opportunity to respond with your own expertise and reasoning. Such conversations
also provide an opportunity to elicit suppressed concerns and a chance
to assure the patient that he or she is part of the process. Noting in
the record a) what the patient requested b) your rationale for denying
that request, and c) what you recommended instead, gives you, the
patient, and subsequent providers context for future requests and
decision making.
Of course, crossing your t’s and dotting your i’s after saying no
doesn’t mean a disgruntled patient won’t pursue a complaint—that’s
beyond your control. But if the complaint is in the form of a
malpractice allegation, then your medical professional liability insurer
will have such claims assessed by medical experts
in your specialty. Their opinion will be based on their own experience,
the prevailing standard of care, and your notes. To that end, a
properly documented decision based on solid clinical judgment and
matched by the practice of your peers is the best support for your
decision to say no.
Additional Material
Original Source, Strategies for Patient Safety
By Jock Hoffman, CRICO
The health care community is experiencing increasing tension between proponents
of evidence-based decision making and dissent driven by provider habits
and patient expectations. Exhibit A is any proposal to scale back
cancer screenings: even those recommendations based on a preponderance
of evidence now instantly face a barrage of counter proposals. Debates
about annual mammograms for women under 50, routine PSA testing, and Pap
tests are just the beginning. Physicians, especially in primary care,
find themselves on the horns of a dilemma: amidst the uproar generated
by political factions, medical societies, patient advocates, and
conspiracy theorists, physicians may well wonder, “Whose advice do I
follow?”
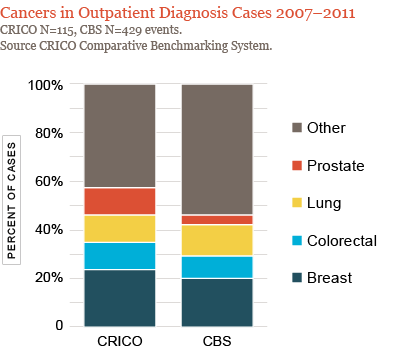
Decision Support from a Malpractice Insurer
Since 1995, CRICO has published and promoted decision support guides
for managing patients through the screening and diagnostic process,
initially for breast cancer, later for colorectal and prostate cancer.
Along with representing three of the four most commonly occurring
cancers, these (plus lung cancer) are those most commonly involved in
failure to diagnose malpractice claims.
CRICO’s primary goal is to help primary care providers assess a
patient’s risk status and need for screening, and to appropriately
manage complaints or symptoms that may indicate the presence of cancer.
In tandem with the risk assessment, the key components of CRICO’s
decision support tools are:
- age and risk stratified screening and intervals between tests;
- recommended steps in response to complaints, symptoms, or abnormal test results;
- triggers for specialty referrals; and
- tips for test results management, coordination of care, and documentation.
To validate its advice for clinical practice, CRICO relies on
accordance between clinical experts from Harvard-affiliated health care
organizations, public agencies, professional societies (and their
respective guidelines), and widely accepted research studies. CRICO’s
process is designed to anchor recommendations in evidence that
withstands time and scrutiny. Each decision support tool is reviewed
every 18–24 months and revised (if necessary) in conjunction with new
evidence and changes in health care delivery practices. In the interim
periods, our expert panels review the literature to determine if they
merit provisional communication with our insured physicians.
CRICO has found that experts from primary care and specialists who
are committed to evidence-based practice develop recommendations that
are credible and practical, especially those that frame the patient’s
decision to undergo testing and those that guide the PCP’s decision to
refer.
Additional Material
Original Source, Strategies for Patient Safety
By Jock Hoffman, CRICO
Through the lens of medical malpractice, the efficacy of PSA testing
is only a sidebar to the factors that prompted someone to allege a
missed diagnosis of prostate cancer. Most often, such cases hinge on how
the test results and the patient were managed by the patient’s primary
care provider (PCP) once PSA testing was initiated. In some instances,
the patient was unaware that a PSA test had been ordered or uniformed of
the results (or both). Here are some recent CRICO data.
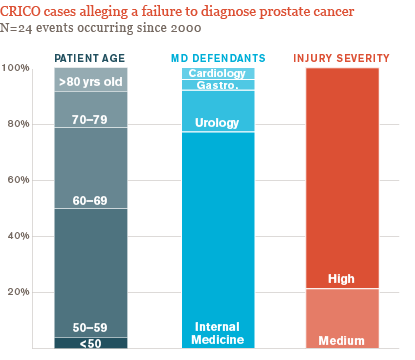 While the debate about PSA testing continues to generate recommendations and counter recommendations,
PCPs can look to a couple of recently closed CRICO malpractice cases
for practical lessons that can reduce the likelihood of being sued by
patients who contend their prostate cancer diagnosis was missed or
delayed.
Of course, it should all begin with a physician-patient discussion about
testing. But once the decision to test has begun, PCPs cannot afford to
leave the follow-up tasks to memory, other providers, or the patient.
Malpractice case studies present an important opportunity for providers
to learn by exploring what went right, what went wrong, and what could
have been done differently. Staff from CRICO’s Patient Safety Department
continually select and develop case studies (of closed claims or
lawsuits) that offer teaching opportunities. More than 80 such case
studies are available on the CRICO web site. Clinician facilitators who
choose to incorporate abstracts from malpractice claims into their
clinical presentations may want to read the suggestions offered in Ten Tips for Presenting Closed Claims Abstracts for Grand Rounds.
While the debate about PSA testing continues to generate recommendations and counter recommendations,
PCPs can look to a couple of recently closed CRICO malpractice cases
for practical lessons that can reduce the likelihood of being sued by
patients who contend their prostate cancer diagnosis was missed or
delayed.
Of course, it should all begin with a physician-patient discussion about
testing. But once the decision to test has begun, PCPs cannot afford to
leave the follow-up tasks to memory, other providers, or the patient.
Malpractice case studies present an important opportunity for providers
to learn by exploring what went right, what went wrong, and what could
have been done differently. Staff from CRICO’s Patient Safety Department
continually select and develop case studies (of closed claims or
lawsuits) that offer teaching opportunities. More than 80 such case
studies are available on the CRICO web site. Clinician facilitators who
choose to incorporate abstracts from malpractice claims into their
clinical presentations may want to read the suggestions offered in Ten Tips for Presenting Closed Claims Abstracts for Grand Rounds.
Additional Material
Original Source, Strategies for Patient Safety
By Jock Hoffman, CRICO
It is a rare discussion among patient safety experts when someone in the room (physician, lawyer, CEO) doesn’t interject, “Let me tell you what happened the last time my mother saw her doctor.”
No matter what our role is in working to perfect patient safety, reduce adverse events, and prevent malpractice claims, we often also get to see systemic imperfections from the patient or family member’s perspective. Indeed, those anecdotes often help build the narratives we use to frame improvement efforts.
One such improvement effort is better coordinated care delivery systems. A recent New York Times article predicted that, by 2020, accountable care organizations (ACOs) and similar care consortiums will have replaced the U.S. health insurance industry. While that’s speculation, providers do need to ramp up their ability to explain new health care delivery models to the patient populations they will be managing. In doing so, those “my mother” patient-perspective narratives become even more poignant for participating physicians.
A key requirement for ACOs and similar entities is more fully engaging patients in their health-related decisions. Exactly how to achieve patient engagement is still a bit murky, but the essential component is enabling patients to conduct well-informed discussions with a coordinated team of providers about their health, care options, and medical decisions. The expected consequence is that patients who appreciate the more focused and synchronized approach to their care will make informed decisions that benefit both themselves and the overall population. An additional benefit is that a more engaged patient population serves as another layer of patient safety protection.
Of course, a patient’s motivation to be engaged in her care can be counterbalanced by skepticism if she doesn’t perceive a direct benefit. Friends, family and the popular media may influence an attitude that patient engagement is just a new tactic for advising everyone to diet and exercise more often. And, even without any external influence, change may engender frustration or distrust for some patients.
For example, decisions regarding what tests are ordered, what consults or referrals are proffered, and what treatment or medications are recommended, may be challenged. Increased access to medical records may introduce unfamiliar terms or information displays that trigger requests for clarification. How you answer your patients’ questions will be a key aspect of their attitudes toward engagement and a healthy physician-patient relationship.
CRICO, and other organizations are working to identify best practices for aligning patient engagement with patient safety. The better that physicians, and the organizations they’re affiliated with, are informed about risks and enabled by proven solutions, the better equipped you’ll be to help “my mother” become an engaged patient.
Additional Material
Original Source, Strategies for Patient Safety
By Jock Hoffman, CRICO
A recently published study measuring the scope of care in an ambulatory practice (Harvard Vanguard Medical Associates) notes that a typical (full-time) general practitioner annually manages more than 1,100 different diagnoses, medications, lab tests, referrals, imaging studies and procedures; some do many more than that. That is both a testament to the complexity of primary care and a yardstick for the risk inherent in a profession that combines so many variables.
Malpractice claims and suits alleging a diagnostic error in a (non-ED) outpatient setting account for 67 percent of all CRICO cases based on care rendered since 2002. Roughly half of those involve cancer, but more than 50 different types; an additional 50 non-cancer diagnoses make up the other half. For 75 diagnosis-related cases involving Emergency Department patients from the same time period, more than 30 different final diagnoses were listed. Clearly, patient safety cannot focus too narrowly on particular case types but, rather, needs to address the potential pitfalls in the diagnostic process for all patients, especially outpatients.
There is, however, value in applying to a broader set of circumstances, generalizable lessons drawn from a subset of high-severity claims, particularly those alleging a failure to diagnose breast, colorectal, or prostate cancer.
Self-detected symptoms
Whether or not you can detect what the patient has indicated (e.g., breast lump, bloody stool, abdominal pain) he or she expects to be followed to conclusion. Leaving a self-detected complaint unresolved (in the patient's mind) may foster distrust. A subsequent diagnosis may be considered "missed" by a patient who believes he or she wasn't taken seriously from the beginning.
Patient risk factors
An insufficient or outdated history (personal and family) can inhibit risk-stratified screening—and timely referrals for high-risk counseling. Patients may need to be prompted and guided through the process of providing an informative history.
Test results
Following an ordered diagnostic test through to a conclusion requires both the ordering physician and other clinicians involved in the process to confirm that it was conducted, and that the results were interpreted, communicated to all pertinent parties, and discussed with the patient. Unconfirmed assumptions put both patient and providers at risk.
Follow-up
A follow-up plan has to become a follow-up action. Documentation, especially when shared with the patient and family members, helps, but only if it is structured with alerts to missed appointments or milestones.
Referrals
A referral treated as a one-way engagement exposes you and your patients to diagnostic delays if anything alters the intended course of events. Make sure to coordinate a closed-loop communication process with clinical colleagues, and clarify for the patient the roles of each of his or her providers.
Managing expectations
Any doubts you have that you will be able to translate a patient's complaint or symptoms or test results into a concrete diagnosis need to be balanced against the patient's expectations. Sharing the limits of the diagnostic process with a patient may help maintain his or her trust during a period of anxiety, and ultimately protect you against an allegation of substandard practice.
Given the vast amount of information patients expect their physicians to learn, retain, and appropriately apply, those physicians who complement their routines and memory with decision support tools are likely to make fewer missteps along the diagnostic path.
Additional Material
Original Source, Strategies for Patient Safety
By Jock Hoffman, CRICO
Health care constantly intersects with challenging decisions, perhaps none more unsettling than the choice between waiting, or acting on an ambiguous presentation. If the patient is not physically present (e.g., on the phone or emailing), then the provider has even fewer cues to guide that decision. When the remote communication of history, symptoms, and status involves third parties (parent, interpreter, answering service, etc.) the risks associated with making a “wait” or “don’t wait” decision increase significantly. Such situations are even further complicated if the patient (or spouse or parent) is hesitant to leave home for the doctor’s office or the nearest emergency room barring a sense of urgency. Physicians and nurses who routinely have remote care encounters are encouraged to review this case study from a recent CRICO malpractice claim.
Malpractice case studies present an important opportunity for providers to learn by exploring what went right, what went wrong, and what could have been done differently. Although these cases often represent negative and emotionally charged circumstances, positive learning can emerge from examining them. Staff from CRICO’s Patient Safety Department continually select and develop case studies (of closed claims or lawsuits) that offer teaching opportunities. More than 75 such case studies are available on the CRICO web site. Clinician facilitators who choose to incorporate abstracts from malpractice claims into their clinical presentations may want to read the suggestions offered in 10 Tips for Presenting Closed Claims Abstracts for Grand Rounds.
Additional Material
Original Source, Strategies for Patient Safety
By Jock Hoffman, CRICO
For virtually every physician-patient interaction, your patient’s past is prologue to today’s encounter and tomorrow’s care plan. But coordination of care—even over a brief office visit or hospital stay—is as much of a patient safety challenge as is making a proper diagnosis or carrying out a successful treatment. The path of care from the initial complaint to completion of treatment is far from seamless. Indeed, it is full of cracks—opportunities for losing, misdirecting, or misunderstanding critical information—that pose serious risks for the patient and his or her multiple health care providers.
Coordination of care risks can derive from patients you see often for chronic care and for those who you’ve never met (e.g., a patient new to your panel being seen in the ED). Most malpractice cases involving poorly coordinated care are those alleging a missed or delayed diagnosis, commonly due to a mismanaged test result, referral, or hand-off. For 522 cases filed against CRICO insureds from January 2005 to October 2010 with care coordination issues, the following three contributing factors were prominent:
- Mismanagement of test results
(234 cases*/average incurred loss=$1M)
- Mismanagement of referral
(230 cases/average incurred loss=$852K)
- Mismanagement of hand-off or sign-out
(255 cases/average incurred loss=$888K)
Those categories comprise myriad communication and documentation factors that prevent multiple caregivers from having a complete picture of the patient’s status and subsequent care needs. Relying solely on memory—yours or the patient’s—is ill-advised; systems that fail to keep everyone (including future providers) well-informed about past care and future responsibilities are equally inadequate.
At the broad level, CRICO is working with its insured organizations to enhance closed-loop communication of test results and referrals, and improve team communication at key transitions for providers (e.g., hand-offs) and patients (e.g., discharge). For individual physicians and nurses, CRICO and its clinical experts have developed answers to a series of Frequently Asked Questions that address many coordination of care issues.
A quick review might help you and your co-providers keep crucial patient information from slipping between the cracks.
*A single malpractice case may involve more than one factor
Additional Material
Original Source, Strategies for Patient Safety

